What is an image-guided biopsy?
An image-guided biopsy aims to provide diagnostic information by obtaining a sample of tissue from under the skin using imaging to navigate. The interventional radiologist will perform this procedure using special cutting needles which are available in a variety of diameters and lengths. The tissue sampled will usually be examined under a microscope by a pathologist and can also be analysed chemically.
How does the procedure work?
If you are on any medication that prevents blood clotting, you will stop taking it before the procedure, if possible.
You should not eat anything for at least four hours before the procedure starts. You may be asked to fast for longer, depending on the puncture and the complexity of your particular case. Before the procedure, the interventional radiologist will usually place a needle in your vein to make access easier during the procedure.
The interventional radiologist may use one of a number of image-guidance techniques to plan and monitor the placement of the needle during the aspiration procedure, including ultrasound, CT, MRI and fluoroscopy. This depends on the location and nature of the lesion.
Most biopsy procedures are performed under local anaesthesia or conscious sedation, so you will be awake but feel no pain. You may be asked to take antibiotics beforehand to reduce the risk of infection, but this is uncommon. You will lie down for the procedure – the exact position you will be asked to lie in depends on the access route that the interventional radiologist will use to safely approach the lesion.
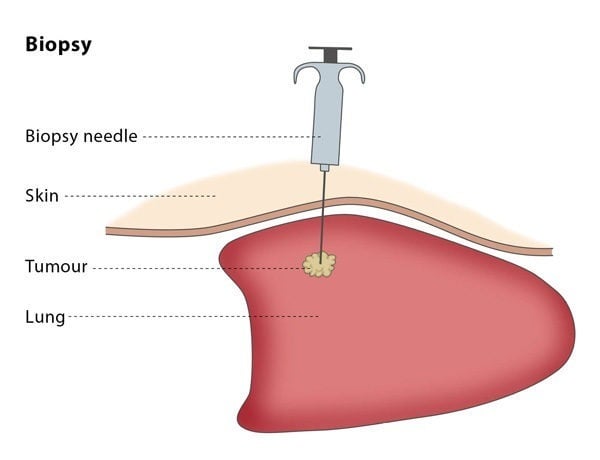
The procedure will be carried out in a sterile and safe environment. The interventional radiologist will choose which type of needle to use according to the organ and tissue type which needs to be sampled, such as bone, soft tissue, lung, etc. The interventional radiologist will insert the needle and will guide it using imaging until the needle tip can be seen inside the lesion.
An image-guided biopsy can be performed as an in-patient or out-patient procedure. The site of the puncture and your vital signs will be monitored for 4-6 hours following the procedure. You will experience some mild discomfort around the puncture site during this time. If you undergo a lung biopsy, you will be given a chest X-ray 6-8 hours after the procedure to ensure that no air has been trapped in the cavity between your chest wall and your lungs. In most cases, you will be allowed to drink water a few hours after the biopsy procedure.
Why perform it?
If you have a lesion and your doctor needs further information to make a diagnosis, you may be referred for an image-guided biopsy.
There are a number of factors which may make the procedure unsuitable for you, including if you have a blood clotting disorder, if there is no safe route for the interventional radiologist to access the lesion, or if you have already been diagnosed using other procedures, such as diagnostic imaging.
The success rate of the biopsy procedure can vary depending on the location of the lesion and the type of needle used. Image guidance is used to confirm that the needle is placed correctly inside the lesion and to help avoid complications.
What are the risks?
If the interventional radiologist uses a small bone needle, the complication rate is low. The most common complications are bruising and infection. If you have had a lung biopsy there is a risk of pneumothorax, which means that air fills the gap between the lungs and the chest wall.
Bibliography
1. Gupta S. Role of image-guided percutaneous needle biopsy in cancer staging. Seminars in Roentgenol 2006; 41(2): 78-90.
2. Kerimaa P, Marttila A, Hyvönen P, et al. MRI-guided biopsy and fine needle aspiration biopsy (FNAB) in the diagnosis of musculoskeletal lesions. Eur J Radiol 2013.
3. Klein JS, Zarka MA. Transthoracic needle biopsy: an overview. J Thorac Imaging 1997; 12(4):232-49.



